Introduction
Some babies are born with a condition called tongue-tie, the medical term for this is ankyloglossia. Tongue-tie affects babies differently, with some not being bothered by it at all, whilst in other babies it may cause feeding difficulties. Baby tongue-tie may be as common as 1 in 10 babies, but not all babies will need to have it treated.
What is tongue-tie?
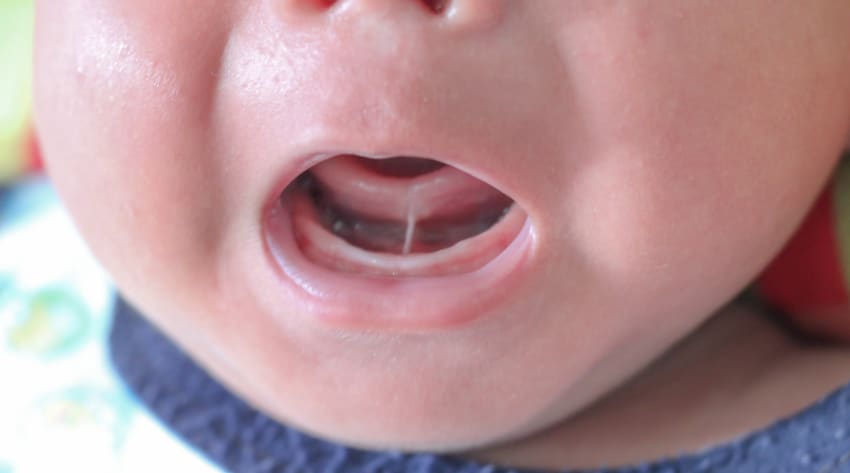
Baby tongue-tie is when the fold of skin under the tongue (called the lingual frenulum) that connects the tongue to the bottom of the mouth is shortened or tight, restricting tongue movement.
There are different types of tongue-tie depending on how the frenulum is affected: Posterior tongue-tie and anterior tongue-tie.
What are the signs of tongue-tie in babies?
Tongue-tie affects both breastfeeding and bottle-feeding. Sometimes you may be able to notice signs of tongue-tie by looking into your baby’s mouth when they’re crying or yawning. Other times, it may not always be so easy to see as it isn’t just about how your baby’s tongue looks; here are some common signs of tongue-tie in baby (and mum):
Tongue tie breastfeeding baby
- Latching on problems during breastfeeding; both difficulty attaching to the breast or staying attached. You may notice your baby frequently comes off the breast or slips back to the nipple
- Frequent and/or long feeds
- Unsettled baby and appearing hungry all the time
- Slower weight gain than expected
- Clicking sound when feeding
- Colic/wind/reflux/hiccups/dribbling
Signs in a breastfeeding mum
- Sore nipples
- Misshapen or discoloured nipples after feeding
- Engorgement, blocked ducts and mastitis (inflammation) can occur if your baby isn’t able to manage a full feed
- Low milk supply
- Long or frequent feeds can be exhausting
- Distress from challenges with establishing breastfeeding
Noticing these signs doesn’t always mean that your baby has a tongue-tie. Your midwife, health visitor or a breastfeeding specialist can help with support and advice on breastfeeding positioning and attachment.
Signs of tongue-tie and bottle feeding
- Baby is slow to take a bottle feed
- Frequent feeding
- Dribbling and/or gagging
- Pushing bottle teat out
- Changing the teat doesn’t help to improve feeding
- Clicking sound when bottle feeding
- Poor weight gain
You may also notice some signs from the way your baby moves their tongue; such as difficulty sticking out their tongue, restricted tongue movement or a heart shaped tongue if they are able to stick out.
How is tongue-tie diagnosed?
Some tongue-ties are easily seen and will be picked up during your baby’s newborn physical examination. Others are not so obvious and may be identified later when feeding issues arise.
Assessment for tongue-tie requires specific training/skills and involves placing a finger in the baby’s mouth. As part of the physical examination, a detailed feeding history should also be taken by the appropriate healthcare professional. If you are breastfeeding your baby then you will also be recommended breastfeeding support from a breastfeeding counsellor or trained breastfeeding professional.
If you have concerns about your baby’s feeding and think they may have tongue-tie, speak to your health visitor, public health nurse, midwife or GP.
How is tongue tie treated?
Tongue-tie treatment is not always needed for every baby. If treatment is recommended then a quick and simple procedure called a tongue-tie division (or known medically as a frenulotomy) is carried out by a specially trained healthcare professional (doctor, nurse, midwife or tongue-tie practitioner). A tongue-tie division releases the tongue so that it can move more freely and your baby will be able to feed straight away after the procedure.
Very young babies do not usually require an anaesthetic (painkiller) and for most babies the treatment does not cause pain. Some babies may cry a little during the procedure, whilst others sleep right through it! You can find out more about tongue-tie treatment here.
Following a tongue-tie division breastfeeding mums report improved breastfeeding (for both baby and mum) and an improved latch. Studies also show improved feeding in bottle-fed babies.
Where can I get help for tongue tie and feeding difficulties
However you are feeding your baby, if you are worried about or need help with feeding, you should speak to your midwife or health visitor for support and advice. If you are breastfeeding then having a complete feed observed by someone specially trained in breastfeeding support can identify ways to help improve feeding for both you and your baby. Advice and support on feeding positions may also help to make things more comfortable for both mum and baby.
What to expect after tongue tie treatment?
A small white blister may appear under your baby’s tongue the day after tongue-tie division. This is quite normal, doesn’t require treatment and should heal in 1-2 days. Some babies show improved feeding immediately, others may take a little longer. It’s important to give yourself and your baby time to get used to feeding once their tongue is able to move more freely.
Does tongue-tie affect speech?
If baby tongue-tie is not treated it may not cause any later problems as a child gets older and any tightness of the tongue may resolve naturally as the mouth develops.
However, sometimes, tongue-tie can affect speech and cause difficulty eating certain foods. If you notice any of these problems please seek advice from your GP.
Next steps
Tongue-tie in babies may not always be the cause of feeding problems, but it is always best to speak to your healthcare professional if you have any concerns or think your baby may have tongue-tie. If you notice any of the signs of tongue-tie, your baby is not gaining weight as expected or you think it would be helpful to get support for feeding your baby, contact a lactation consultant. If you do not have access to a lactation consultant, you can contact your infant feeding specialist, midwife, public health nurse, GP, neonatologist, or paediatrician.

Midwife Live Chat
We have partnered with Epical Global giving our SMA® Baby Club members instant access to a team of expert midwives, ready to answer all your questions. The midwife team are on hand via live chat Monday to Friday, 10am – 8pm.
Feeding issues symptom checker
Experiencing feeding issues with your newborn?
Get help narrowing down the cause with our symptom checker.